The Human Papillomavirus: Understanding its Impact and Prevention
The Human Papillomavirus (HPV) represents the most prevalent sexually transmitted infection globally, affecting millions of individuals regardless of age, gender, or sexual orientation. Estimates from health authorities indicate that nearly 80% of individuals will encounter this virus at some point in their lives, leading to a range of health outcomes. Despite its widespread nature, the conversation surrounding HPV remains shrouded in misinformation and stigma, which complicates prevention efforts. This article seeks to clarify what HPV truly is, how it spreads, its potential health consequences, and most importantly, how one can effectively prevent it.
What Exactly is HPV?
HPV is not a singular virus; rather, it constitutes a group of over 100 distinct types of viruses, each affecting the skin and mucosal surfaces. Categorizing HPV is primarily based on its potential to cause cancer, leading to a division into two main types: low-risk HPV and high-risk HPV.
Low-risk HPV types are chiefly linked to benign conditions, such as genital warts and mild cellular alterations, which typically do not progress to cancer. For instance, HPV types 6 and 11 are responsible for around 90% of genital warts cases. Conversely, high-risk HPV includes approximately 15 strains identified as oncogenic, significantly associated with various cancers. The most notorious among these is cervical cancer, but it can also lead to malignancies in other areas, including the anus, penis, vulva, vagina, and oropharynx. Understanding these distinctions is crucial for effective prevention and treatment strategies.
Dispelling Common Myths About HPV
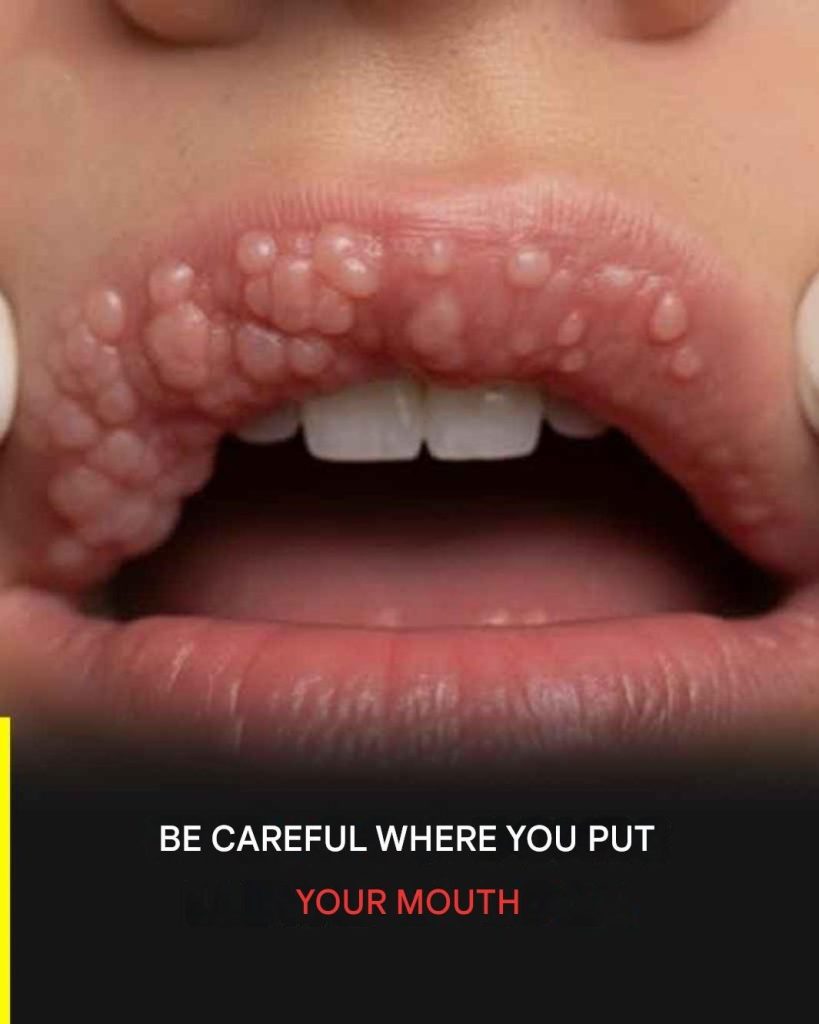
Despite the growing awareness surrounding HPV, numerous myths continue to flourish, complicating prevention efforts. One prevalent misconception is that HPV only affects women. This is far from the truth—both men and women are susceptible to the virus, and men can experience serious health consequences, including cancers linked to HPV. In many cases, men may carry and transmit HPV without ever displaying symptoms, making the virus a silent threat.Another common myth involves the belief that HPV can be transmitted through casual contact—such as sharing towels, using public restrooms, or swimming pools. In reality, HPV is transmitted exclusively through direct skin-to-skin contact during sexual activities, which include vaginal, anal, and oral sex. This highlights the importance of understanding safe practices in sexual health, emphasizing the need for open discussions about HPV and its transmission.
A particularly dangerous belief is that if one does not exhibit symptoms, they are free from infection. In fact, the majority of individuals infected with HPV remain asymptomatic, allowing the virus to spread unknowingly. This underscores the necessity for regular health check-ups and awareness about HPV, as many individuals may unknowingly pass the virus to their partners.
HPV and Its Connection to Cancer
HPV stands as the leading cause of cervical cancer, a devastating disease that affects women worldwide. Alarmingly, it is estimated that nearly 99% of cervical cancer cases can be traced back to an HPV infection. In regions such as Latin America, the most prevalent strains linked to cervical lesions include HPV 16, found in 53.2% of cases, and HPV 18, noted in 13.2%. Cervical cancer ranks as the third most common cancer among women globally and represents a significant cause of cancer mortality in young women, with approximately 4,600 new cases diagnosed annually in Argentina alone. This stark statistic highlights the urgent need for effective prevention strategies.
Yet, the implications of HPV extend beyond cervical cancer. Both men and women face the risk of developing other malignancies, such as anal, penile, vulvar, vaginal, and oropharyngeal cancers. The broad spectrum of potential cancer types associated with HPV necessitates a comprehensive understanding and proactive measures. For example, oropharyngeal cancers are on the rise, particularly among men, and can be attributed to certain high-risk HPV strains, showcasing the virus’s far-reaching impact.
Effective Prevention Strategies for HPV
While there is no definitive cure for HPV itself, its repercussions can be significantly mitigated through various preventive strategies. Prevention is typically classified into two main categories: primary prevention and secondary prevention.
Primary prevention focuses on thwarting infection before it occurs. Two paramount measures in this regard include:
Comprehensive Sexuality Education (CSE): Providing individuals, especially the youth, with accurate information regarding sexual and reproductive health is vital for reducing the transmission of HPV and other sexually transmitted infections. Programs that educate young people about HPV, its risks, and safe practices help create informed communities less susceptible to misinformation.
Vaccination: The HPV vaccine, included in national immunization schedules, is administered free of charge to 11-year-old girls and boys and is also available to other at-risk demographics. This vaccine is instrumental in protecting against the most dangerous strains of HPV, significantly diminishing the risk of developing cancer linked to the virus. Studies have shown that vaccination rates correlate with a decline in HPV-related cancers, underscoring its importance.