An In-Depth Look at Psoriasis: Understanding Types, Causes, and Treatments
Psoriasis is a chronic skin condition impacting millions of individuals globally, with varying degrees of severity and manifestations. Understanding this multifaceted disorder is crucial for those affected, as it allows for better management and improved quality of life. This article aims to provide an extensive overview of psoriasis, exploring its various types, underlying causes, common triggers, diagnostic practices, and treatment options available. By gaining insights into this condition, patients can take proactive steps toward managing their symptoms effectively.
Types of Psoriasis
Psoriasis is classified into five primary types, each presenting unique symptoms, challenges, and treatment considerations. Recognizing these variations is essential for effective management.
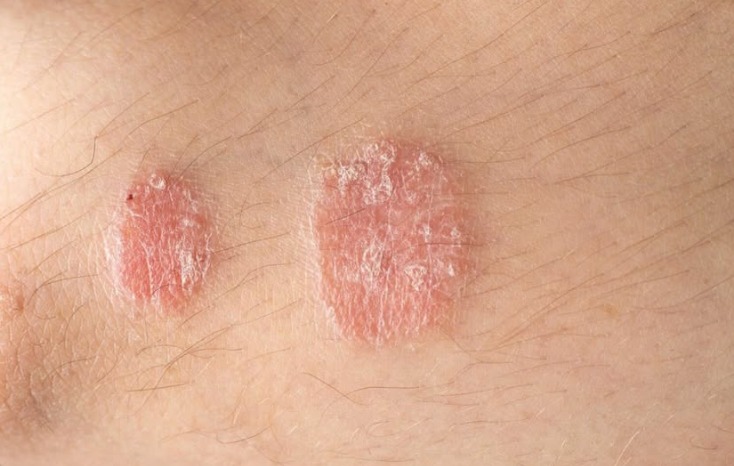
Plaque Psoriasis stands out as the most prevalent form, affecting around 80-90% of individuals diagnosed with psoriasis. This type is characterized by raised, red patches covered with thick, silvery scales. Commonly found on the elbows, knees, scalp, and lower back, plaque psoriasis can lead to considerable itching and discomfort, potentially hindering daily activities. The plaques can also become inflamed and painful, leading to further complications if not treated appropriately.
In contrast, Guttate Psoriasis is noted for its distinctive drop-shaped lesions, which often appear suddenly and can be triggered by bacterial infections, particularly streptococcal throat infections. This type is more frequently observed in children and young adults, making it particularly concerning for parents of those affected. The lesions can cover large areas and significantly impact skin appearance, leading to emotional distress for those afflicted.
Pustular Psoriasis, another variant, is marked by white pustules (blisters) filled with non-infectious pus, surrounded by red, inflamed skin. This type may appear in localized areas, such as the hands and feet, or may be widespread across the body. The pustules can be incredibly painful and lead to significant discomfort, making daily tasks a challenge.
Inverse Psoriasis is characterized by bright red, shiny lesions that develop in skin folds, like the armpits, groin, and under the breasts. This type often causes friction and irritation due to the areas in which it occurs, leading to additional discomfort. Inverse psoriasis can also be challenging to diagnose and treat, as traditional psoriasis treatments may not be effective in these moisture-rich environments.
Lastly, Erythrodermic Psoriasis represents a rare and severe form of the disease, causing widespread inflammation and exfoliation over a significant portion of the body. This emergency condition can disrupt the body’s thermoregulation, leading to severe complications if not treated immediately. Patients experiencing erythrodermic psoriasis often require hospitalization and intensive medical intervention to stabilize their condition.
Causes and Triggers of Psoriasis
The causes of psoriasis are complex and largely associated with immune system dysfunction. In individuals with psoriasis, T-cells—specific types of white blood cells—mistakenly target healthy skin cells, prompting an accelerated production of skin cells. This rapid turnover leads to the accumulation of dead skin cells and the formation of scaly plaques.
Genetic predisposition plays a significant role in the development of psoriasis. Studies indicate that if a close family member has psoriasis, the likelihood of developing the condition increases substantially. Approximately one-third of patients report having a family history of psoriasis, highlighting the importance of genetic factors in the disease’s manifestation.
Environmental triggers further complicate the condition. Stress is one of the most common exacerbating factors, with studies suggesting that heightened emotional stress can lead to flare-ups. Other triggers include alcohol consumption, smoking, certain medications (like beta-blockers and lithium), and infections, particularly throat infections. Physical trauma, such as cuts or scrapes, may also trigger new lesions, emphasizing the need for individuals to monitor and identify their personal triggers.
Diagnosis of Psoriasis
Diagnosing psoriasis typically begins with a comprehensive physical examination conducted by a qualified healthcare professional. The physician will evaluate the appearance of the skin, often considering the distribution and type of lesions present. Patients are usually asked about their medical history, family history of skin conditions, and any symptom patterns they’ve experienced.
In certain cases, a skin biopsy may be performed to confirm the diagnosis. This procedure involves removing a small sample of skin to be examined under a microscope, helping to distinguish psoriasis from other skin disorders, such as eczema or fungal infections. This step is critical in ensuring that an accurate diagnosis is made, allowing for the implementation of the most effective treatment strategy.
Treatment Options for Psoriasis
While there is currently no definitive cure for psoriasis, a variety of treatment options are available to help manage symptoms and enhance the quality of life for those affected. Treatment plans are often tailored to the severity of the condition and the specific type of psoriasis diagnosed. Topical treatments generally serve as the first line of defense, employing medications such as corticosteroids, vitamin D analogs, and retinoids. These topical agents work to reduce inflammation, alleviate scaling, and promote skin cell turnover.
For moderate to severe cases, patients may require systemic treatments, which are administered orally or injected and impact the entire body. These treatments include methotrexate, cyclosporine, and biologics—advanced therapies that specifically target components of the immune system. Biologics, in particular, have revolutionized the psoriasis treatment landscape, offering targeted relief and improved outcomes for many patients, especially those who have not responded well to traditional therapies.
Another effective treatment option is phototherapy, which involves exposing the skin to ultraviolet (UV) light under professional supervision. This method is particularly beneficial for individuals who do not respond favorably to topical treatments alone. Phototherapy can help slow down the rapid skin cell production associated with psoriasis, but it requires ongoing treatment to maintain results.
Living with Psoriasis
Living with psoriasis presents numerous challenges, both physical and emotional. Many individuals contend with feelings of self-consciousness and stigma linked to visible skin lesions, which can have a profound impact on mental health. Emotional support from healthcare providers, support groups, and family can be crucial in navigating the complexities of living with this chronic condition.
Maintaining a healthy lifestyle is imperative for managing psoriasis effectively. Regular exercise, a balanced diet, and mindfulness practices can significantly enhance the effectiveness of treatment plans and improve overall well-being. Additionally, avoiding known triggers—such as excessive alcohol consumption, smoking, and unmanaged stress—can further support individuals in managing their symptoms effectively.
In conclusion, while psoriasis remains a lifelong condition that presents unique challenges, understanding its various types, underlying causes, and treatment options empowers individuals to take control of their health. Through education, proactive management strategies, and a strong support network, those living with psoriasis can lead fulfilling, active lives. Encouraging awareness and reducing stigma around psoriasis is essential for fostering a supportive environment for all affected by this condition.