The Mystery of Paresthesia: Why Do Our Limbs “Fall Asleep”?
Have you ever experienced the uncomfortable sensation of your limbs falling asleep? You know the feeling—a dull numbness that is often accompanied by a tingling or prickling sensation, colloquially referred to as “pins and needles.” This phenomenon is medically known as paresthesia, and it occurs when specific areas of the body temporarily lose sensation. But what triggers this peculiar sensation? In this article, we delve into the science behind paresthesia, exploring its causes, implications, and prevention strategies. Understanding the complexities of paresthesia is not just about grasping a transient feeling; it opens a window into our nervous system’s functioning and our overall health.
Understanding Paresthesia: What Happens When We “Fall Asleep”?
Paresthesia manifests as a tingling or prickling sensation, and it often affects the extremities—namely the hands, arms, legs, and feet. When we describe a body part as having “fallen asleep,” it generally indicates that nerve pathways are being disrupted. This disruption can happen due to pressure on a nerve, which interferes with its ability to send signals to the brain. Consequently, this leads to sensations of numbness and tingling. The physiological process involves the complex interplay between the nerves and the blood vessels that supply them. When a nerve is compressed, it can cause a temporary loss of proprioception—the body’s ability to perceive its position in space, which is crucial for coordination and movement.
Common Triggers of Paresthesia
Paresthesia can arise from a variety of circumstances, often categorized into three primary causes:
Nerve Compression
One of the most prevalent reasons for paresthesia is nerve compression. This occurs when a nerve is pinched or compressed, interrupting its ability to function properly. Common scenarios include:
- Sleeping with an arm tucked beneath your head
- Sitting cross-legged for extended periods
- Remaining in a single position for too long, such as during long car rides or while working at a desk
When you change positions, the pressure on the nerve is alleviated, and normal sensation tends to return quickly. However, repeated instances of this can lead to chronic issues, as persistent nerve compression can result in long-term damage to the nerve pathways if not addressed promptly.
Circulatory Issues
Circulation can also play a significant role in causing paresthesia. If blood vessels are compressed, the affected area may not receive an adequate supply of oxygen and essential nutrients. This insufficient blood flow can lead to a temporary sensation of numbness. For example, if you’ve ever sat for too long in a cramped airplane seat and then felt tingling in your legs, it’s likely due to circulation issues. Fortunately, once you shift your position and restore proper circulation, the tingling usually disappears. Yet, chronic circulatory problems can have more severe implications, such as increasing the risk of vascular diseases.
Underlying Medical Conditions
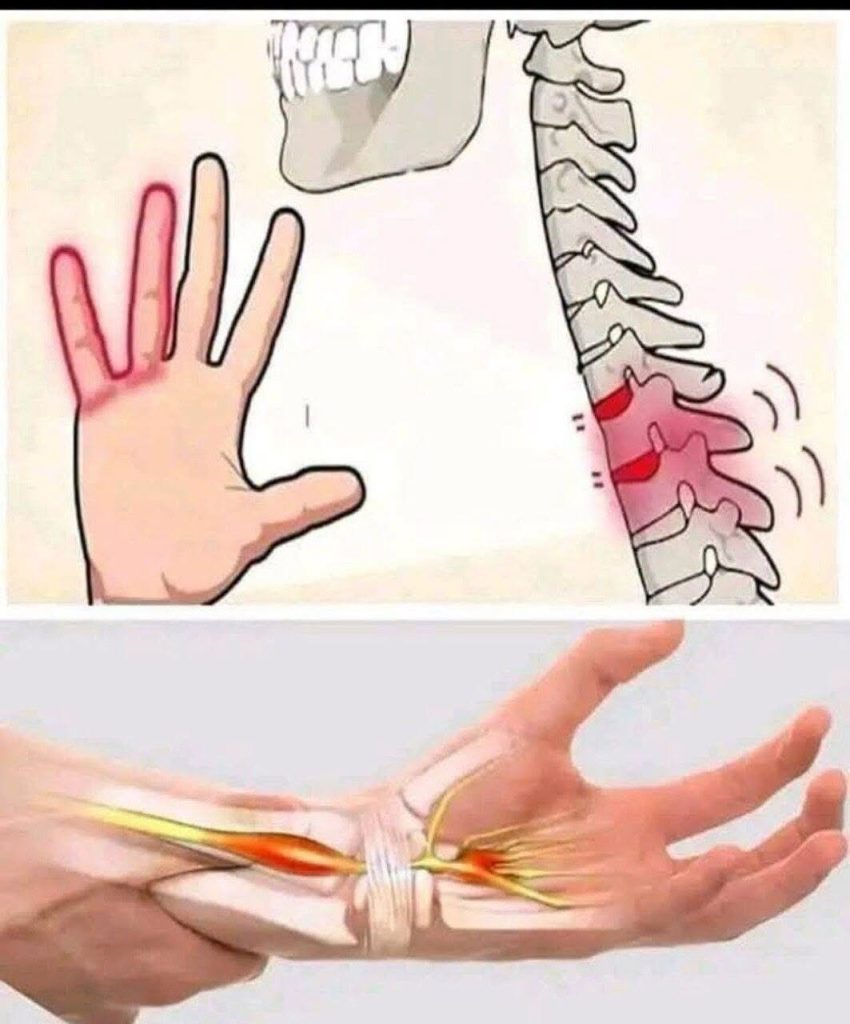
While occasional paresthesia is generally benign, recurring or persistent symptoms may signal underlying medical conditions. Notable health issues associated with chronic paresthesia include:- Carpal Tunnel Syndrome: This syndrome results from the median nerve being compressed as it passes through the wrist, leading to persistent tingling and numbness in the hand, particularly among those who perform repetitive tasks. For instance, writers and typists may be particularly at risk.
- Diabetes: Diabetic neuropathy can lead to nerve damage, causing numbness and tingling in various parts of the body, often starting in the feet. This condition can significantly impact the quality of life, making it crucial for individuals with diabetes to manage their blood sugar levels.
- Multiple Sclerosis (MS): This autoimmune disorder can affect nerve cells in the brain and spinal cord, often leading to unusual sensations, including paresthesia. Symptoms can vary widely from person to person, complicating diagnosis and treatment.
- Spinal Issues: Herniated discs or spinal stenosis may compress nerves in the back, causing numbness in the extremities. Individuals with back pain should be aware of this as it may be indicative of larger problems.
The Science Behind the Disappearance of Sensation
Why does the tingling sensation often fade away after a movement? In most cases, the discomfort is temporary. Once you change positions, the pressure on the affected nerve or blood vessel is relieved, allowing normal blood flow to be restored. As blood circulation resumes, the nerves “wake up,” leading to the prickling sensation that accompanies the return of feeling. This phenomenon is typically harmless but may signal the need for better posture or more frequent movement if it occurs regularly. The body is remarkably resilient, but it does require our attention to maintain proper function.